Arthroscopic ACL Reconstruction
What is the Anterior Cruciate Ligament?
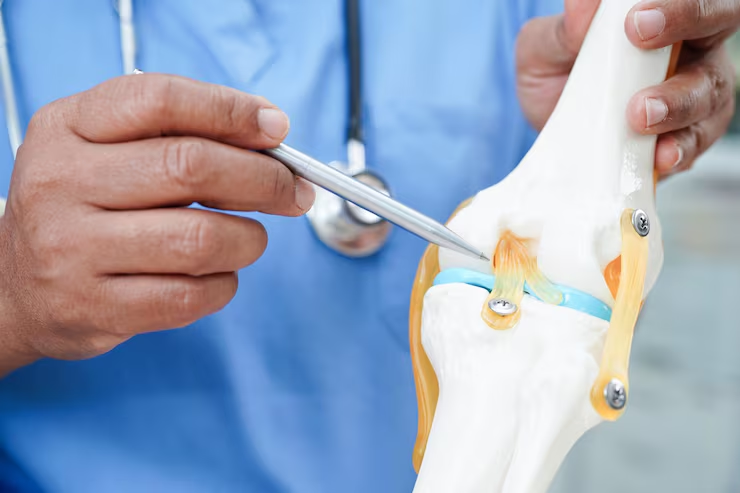
Torn ACL
- Improved knee stability
- Improved mobility
- Reduced pain
- Full recovery of function and return to sport

What is ACL reconstruction surgery?
The operation involves using part of either your hamstring tendons (from the back of your knee) or the middle third of your patella tendon (from the front of the knee just below your knee cap) to replace the torn ACL inside your knee joint. Your surgeon will have discussed with you which type of graft is to be used in your case. This is dependent on a number of factors such as your sex, build, and the type of sport you play.
Hamstring graft
During a hamstring reconstruction a small incision (cut) is made over the inner part of your knee to harvest (remove) two of your hamstring tendons to use for your graft. They are braided together to form a new ligament. The graft is placed in tunnels drilled into the tibia and femur and fixed into the knee with a special button at the top and a screw at the bottom, matching the original position of the ruptured ligament. You will also have two very small incisions – one on either side, just below your kneecap for the surgical instruments and camera to see inside your knee; and a small incision on the outside of the lower thigh to assist the placement of the graft on the upper part of the knee joint.
ACL Graft in Situ
For both types of surgery the keyhole camera (arthroscope) is used to check the whole of the knee joint for signs of wear and tear and attend to any cartilage damage.
The wounds are normally closed with clips or dissolvable stitches and steri-strips, covered with simple dressings, and bandaged with a wool and crepe bandage to keep the swelling to a minimum for the first 24-48 hours. Depending on your muscle control you may also have a knee splint in place for 24 hours to help stabilise the joint and protect the graft until your muscle function returns.
What are the risks?
All operations involve an element of risk:
- Potential problems for ACL reconstruction include graft re-rupture and joint stiffness.
- Uncommon problems include infection, and blood clot (otherwise known as a Deep Vein Thrombosis or DVT).
- Rare problems include nerve or blood vessel
- Minor complications relating to the anaesthetic such as sickness and nausea are relatively common. Heart, lung or neurological problems are much
Please discuss these issues with the doctor if you would like further information.
Before Surgery
The condition of your knee before surgery is important to your recovery after surgery. Ideally, your knee should be in as normal a state as possible other than having a torn ACL. Although you may have some instability you should aim to have:
Little or no swelling
Full range of knee movement
Good lower limb strength and control (around the knee and hip)
Normal walking pattern
Frequently Asked Questions
Will it be painful?
Although you will only have small scars, this procedure can be painful because of the surgery performed inside your knee. The following pain control methods are used to ensure you have as little discomfort as possible:
- Local anaesthetic injection into the wound immediately after the operation
- Painkillers and anti-inflammatory medication taken regularly
- Ice application
Local anaesthetic injection
This is used to decrease the pain in the knee joint and the incision area immediately after your operation which can:
- Reduce the risk of feeling sick or vomiting
- Allow you to eat and drink earlier
- Enable you to get up and mobilise earlier
- Lessen the chance of an overnight stay in hospital
Painkillers
You will be given painkillers (either as tablets or injections) to help reduce the discomfort whilst you are in hospital. A one week prescription for continued pain medication will be given to you for your discharge home. Keep the pain under control by using the medication regularly at first. It is important to keep the pain to a minimum as this will enable you to move the knee more easily, recover muscle function in your thigh muscles, and begin the exercises you will be given by the physiotherapist.
Ice
If you do not have any circulatory disorders, you will benefit from applying ice regularly following surgery. This will help to minimise pain and swelling. Firstly wrap the knee with cling film when applying prior to your wound having healed. Then place a bag of frozen peas, ice cubes, or an ice pack in a damp tea towel. Elevate your affected leg and apply your ice pack for approximately 20 minutes. This should be done regularly throughout the day.
Will I need to use crutches?
Do I need to do exercises?
What do I do about the wound?
When you are discharged from hospital you will have a compression bandage on your knee that should remain in place for 24-48 hours. After this time, remove the bandage and change the small plaster dressings underneath if they are blood stained. You must take extra care to ensure you have thoroughly washed your hands to prevent infection before you change the dressings.
It is important to keep your wound clean and dry until it is fully healed. Stitches, clips or steri-strips may need removing which is usually carried out between 10 and 14 days after your operation. The ward staff will inform you about how to get them removed. They may send a referral to your GP or you may be instructed to go to your GP to arrange this yourself. Alternatively, this may be done at your first clinic visit. The wound should remain covered with the dressings until the stitches, clips or steri-strips are removed.
You may shower before the removal of the stitches/clips/steri-strips – you will need to put several layers of cling film around your knee to keep the area dry. Pat the area when drying yourself and do not rub over the wound sites. Be guided by the clinician who
removes your stitches/clips/steri-strips as to when you can stop using cling film and leave the wound uncovered.
Is there anything I need to watch out for?
You may notice some sensation loss around your wound. This is normal. The area will shrink in size but you may experience a small area of numbness permanently.
Occasionally problems do occur. Signs of possible problems include:
- Increased knee pain not reduced by medication, dramatic increase in knee swelling, inability to weight-bear – this could indicate an infection and you should attend accident and emergency as soon as
- Marked calf pain or swelling and swelling around the ankle – this could indicate a blood clot (DVT) and you should attend accident and emergency as soon as
- Increased temperature. It is normal to have a slight fever following surgery but anything more or that lasts may indicate a
- Stomach upset after taking
- Increased loss of knee
Unless otherwise stated, if you experience any of these problems in your first week please contact your GP or one of our team.
When do I return to the outpatient clinic?
An appointment is usually arranged for 2-3 weeks after you are discharged from hospital to check your progress. Please discuss any queries or worries you may have when you are at the clinic. Appointments are made after this as necessary.
If you have not received an appointment it is essential you phone the outpatient department.
Your physiotherapy appointments should begin within one week of your operation and these will continue for several months until you are able to return to your normal pre-injury activities.
Are there things I should avoid doing?
o protect your new graft you will need to avoid putting too much stress through it. You should not perform any twisting, turning or pivoting manoeuvres on your affected leg. You should also avoid straightening the leg out when you are in a sitting position i.e. a leg extension exercise.
You should avoid standing for prolonged periods of time as this will increase the swelling in your knee. If your knee is swollen you will need to elevate your leg and use ice as instructed.
It is important to avoid walking with a limp – use crutches if needed to allow you to put the weight through your leg in the correct manner i.e. walking with the heel going down first, and also not walking on a bent knee.
When can I drive?
You may drive when you are comfortable and safe to do so. You must have stopped using crutches, be able to sit comfortably and have enough power and bend in your knee to perform an emergency stop. The law states that you should be in complete control of your car at all times. It is your responsibility to ensure this and to inform your insurance company about your surgery. Please ask your physiotherapist for advice
When can I return to work?
When can I fly?
It is recommended that you do not fly for six weeks after the surgery.
How will I progress?
During your first visit after surgery your physiotherapist will decide how often they would like to see you depending on your progress. Initially you may need regular appointments to help and support you through the early stages of rehabilitation. You will be given exercises to perform at home and in the gym and you may progress to a gym-based class at the physiotherapy department.
It is extremely important that you continue to work on the exercise programme you are given and follow your physiotherapist’s instructions carefully.
Your return to leisure activities will be guided by your physiotherapist and will depend on how you are progressing and whether you are reaching certain goals. Your therapist will advise you when you are physically capable of dealing with different activities and will ensure you progress to a level where it is safe for you to return to sport.
The earliest return to sport is 6 months after your operation but this will vary depending on your progress. It is extremely important that you take guidance on this by your physiotherapist, as if you return too early you may not achieve a good outcome from your surgery, and you have a greater chance of your reconstruction failing.

